VIVO Pathophysiology
Control of Thyroid Hormone Synthesis and Secretion
The chief stimulator of thyroid hormone synthesis is thyroid-stimulating hormone from the anterior pituitary. Binding of TSH to receptors on thyroid epithelial cells seems to enhance all of the processes necessary for synthesis of thyroid hormones, including synthesis of the iodide transporter, thyroid peroxidase and thyroglobulin.
The magnitude of the TSH signal also sets the rate of endocytosis of colloid - high concentrations of TSH lead to faster rates of endocytosis, and hence, thyroid hormone release into the circulation. Conversely, when TSH levels are low, rates of thyroid hormone synthesis and release diminish.
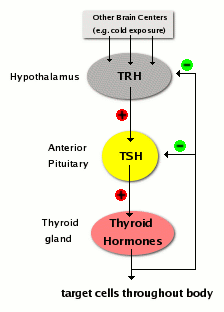
The thyroid gland is part of the hypothalamic-pituitary-thyroid axis, and control of thyroid hormone secretion is exerted by classical negative feedback, as depicted in the diagram. Thyroid-releasing hormone (TRH) from the hypothalamus stimulates TSH from the pituitary, which stimulates thyroid hormone release. As blood concentrations of thyroid hormones increase, they inhibit both TSH and TRH, leading to "shutdown" of thyroid epithelial cells. Later, when blood levels of thyroid hormone have decayed, the negative feedback signal fades, and the system wakes up again.
A number of other factors have been shown to influence thyroid hormone secretion. In rodents and young children, exposure to a cold environment triggers TRH secretion, leading to enhanced thyroid hormone release. This makes sense considering the known ability of thyroid hormones to spark body heat production.
Send comments to Richard.Bowen@colostate.edu

