VIVO Pathophysiology
Endocrine Control of Calcium and Phosphate Homeostasis
It would be very difficult to name a physiologic process that does not depend, in one way or another, on calcium. It is critical to maintain blood calcium concentrations within a tight normal range. Deviations above or below the normal range frequently lead to serious disease.
- Hypocalcemia refers to low blood calcium concentration. Clinical signs of this disorder reflect increased neuromuscular excitability and include muscle spasms, tetany and cardiac dysfunction.
- Hypercalcemia indicates a concentration of blood calcium higher than normal. The normal concentration of calcium and phosphate in blood and extracellular fluid is near the saturation point; elevations can lead to diffuse precipitation of calcium phosphate in tissues, leading to widespread organ dysfunction and damage.
Preventing hypercalcemia and hypocalcemia is largely the result of robust endocrine control systems.
Body Distribution of Calcium and Phosphate
There are three major pools of calcium in the body:
- Intracellular calcium: A large majority of calcium within cells is sequestered in mitochondria and endoplasmic reticulum. Intracellular free calcium concentrations fluctuate greatly, from roughly 100 nM to greater than 1 uM, due to release from cellular stores or influx from extracellular fluid. These fluctuations are integral to calcium's role in intracellular signaling, enzyme activation and muscle contractions.
- Calcium in blood and extracellular fluid: Roughly half of the calcium in blood is bound to proteins. The concentration of ionized calcium in this compartment is normally almost invariant at approximately 1 mM, or 10,000 times the basal concentration of free calcium within cells. Also, the concentration of phosphorus in blood is essentially identical to that of calcium.
- Bone calcium: A vast majority of body calcium is in bone. Within bone, 99% of the calcium is tied up in the mineral phase, but the remaining 1% is in a pool that can rapidly exchange with extracellular calcium.
As with calcium, the majority of body phosphate (approximately 85%) is present in the mineral phase of bone. The remainder of body phosphate is present in a variety of inorganic and organic compounds distributed within both intracellular and extracellular compartments. Normal blood concentrations of phosphate are very similar to calcium.
Fluxes of Calcium and Phosphate
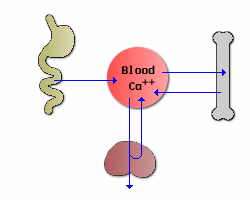
Maintaining constant concentrations of calcium in blood requires frequent adjustments, which can be described as fluxes of calcium between blood and other body compartments. Three organs participate in supplying calcium to blood and removing it from blood when necessary:
|
 |
Hormonal Control Systems
Maintaining normal blood calcium and phosphorus concentrations is managed through the concerted action of three hormones that control fluxes of calcium in and out of blood and extracellular fluid:
Parathyroid hormone serves to increase blood concentrations of calcium. Mechanistically, parathyroid hormone preserves blood calcium by several major effects:
- Stimulates production of the biologically-active form of vitamin D within the kidney.
- Facilitates mobilization of calcium and phosphate from bone. To prevent detrimental increases in phosphate, parathyroid hormone also has a potent effect on the kidney to eliminate phosphate (phosphaturic effect).
- Maximizes tubular reabsorption of calcium within the kidney. This activity results in minimal losses of calcium in urine.
Vitamin D acts also to increase blood concentrations of calcium. It is generated through the activity of parathyroid hormone within the kidney. Far and away the most important effect of vitamin D is to facilitate absorption of calcium from the small intestine. In concert with parathyroid hormone, vitamin D also enhances fluxes of calcium out of bone.
Calcitonin is a hormone that functions to reduce blood calcium levels. It is secreted in response to hypercalcemia and has at least two effects:
- Suppression of renal tubular reabsorption of calcium. In other words, calcitonin enhances excretion of calcium into urine.
- Inhibition of bone resorption, which would minimize fluxes of calcium from bone into blood.
Although calcitonin has significant calcium-lowing effects in some species, it appears to have a minimal influence on blood calcium levels in humans.
A useful way of looking at how hormones affect tissues to preserve calcium homeostasis is to examine the effects of calcium deprivation and calcium loading. The following table summarizes body responses to conditions that would otherwise lead to serious imbalances in calcium and phosphate levels in blood.
| Calcium Deprivation | Calcium Loading | |
|---|---|---|
| Parathyroid hormone | Secretion stimulated | Secretion inhibited |
| Vitamin D | Production stimulated by increased parathyroid hormone secretion | Synthesis suppressed due to low parathyroid hormone secretion |
| Calcitonin | Very low level secretion | Secretion stimulated by high blood calcium |
| Intestinal absorption of calcium | Enhanced due to activity of vitamin D on intestinal epithelial cells | Low basal uptake |
| Release of calcium and phosphate from bone | Stimulated by increased parathyroid hormone and vitamin D | Decreased due to low parathyroid hormone and vitamin D |
| Renal excretion of calcium | Decreased due to enhanced tubular reabsorption stimulated by elevated parathyroid hormone and vitamin D; hypocalcemia also activates calcium sensors in loop of Henle to directly facilitate calcium reabsorption | Elevated due to decreased parathyroid hormone-stimulated reabsorption. |
| Renal excretion of phosphate | Strongly stimulated by parathyroid hormone; this phosphaturic activity prevents adverse effects of elevated phosphate from bone resorption | Decreased due to hypoparathyroidism |
| General Response | Typically see near normal serum concentrations of calcium and phosphate due to compensatory mechanisms. Long term deprivation leads to bone thining (osteopenia). | Low intestinal absorption and enhanced renal excretion guard against development of hypercalcemia. |
| Summary | 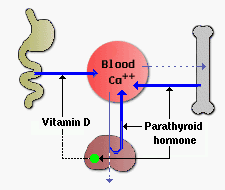 |
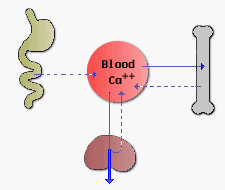 |
Send comments to Richard.Bowen@colostate.edu
