VIVO Pathophysiology
Gonadotropins: Luteinizing and Follicle Stimulating Hormones
Luteinizing hormone (LH) and follicle-stimulating hormone (FSH) are called gonadotropins because stimulate the gonads - in males, the testes, and in females, the ovaries. They are not necessary for life, but are essential for reproduction. These two hormones are secreted from cells in the anterior pituitary called gonadotrophs. Most gonadotrophs secrete only LH or FSH, but some appear to secrete both hormones.
As described for thyroid-simulating hormone, LH and FSH are large glycoproteins composed of alpha and beta subunits. The alpha subunit is identical in all three of these anterior pituitary hormones, while the beta subunit is unique and endows each hormone with the ability to bind its own receptor.
Physiologic Effects of Gonadotropins
Physiologic effects of the gonadotrophins are known only in the ovaries and testes. Together, they regulate many aspects of gonadal function in both males and females.
Luteinizing Hormone
In both sexes, LH stimulates secretion of sex steroids from the gonads. In the testes, LH binds to receptors on Leydig cells, stimulating synthesis and secretion of testosterone. Theca cells in the ovary respond to LH stimulation by secretion of testosterone, which is converted into estrogen by adjacent granulosa cells.
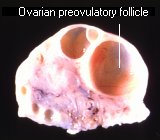
In females, ovulation of mature follicles on the ovary is induced by a large burst of LH secretion known as the preovulatory LH surge. Residual cells within ovulated follicles proliferate to form corpora lutea, which secrete the steroid hormones progesterone and estradiol. Progesterone is necessary for maintenance of pregnancy, and, in most mammals, LH is required for continued development and function of corpora lutea. The name luteinizing hormone derives from this effect of inducing luteinization of ovarian follicles.
Follicle-Stimulating Hormone
As its name implies, FSH stimulates the maturation of ovarian follicles. Administration of FSH to humans and animals induces "superovulation", or development of more than the usual number of mature follicles and hence, an increased number of mature gametes.
FSH is also critical for sperm production. It supports the function of Sertoli cells, which in turn support many aspects of sperm cell maturation.
Control of Gonadotropin Secretion
The principle regulator of LH and FSH secretion is gonadotropin-releasing hormone (GnRH, also known as LH-releasing hormone). GnRH is a ten amino acid peptide that is synthesized and secreted from hypothalamic neurons and binds to receptors on gonadotrophs.
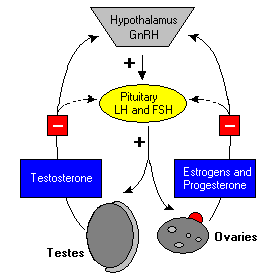
As depicted in the figure to the right, GnRH stimultes secretion of LH, which in turn stimulates gonadal secretion of the sex steroids testosterone, estrogen and progesterone. In a classical negative feedback loop, sex steroids inhibit secretion of GnRH and also appear to have direct negative effects on gonadotrophs.
This regulatory loop leads to pulsatile secretion of LH and, to a much lesser extent, FSH. The number of pulses of GnRH and LH varies from a few per day to one or more per hour. In females, pulse frequency is clearly related to stage of the cycle.
Numerous hormones influence GnRH secretion, and positive and negative control over GnRH and gonadotropin secretion is actually considerably more complex than depicted in the figure. For example, the gonads secrete at least two additional hormones - inhibin and activin - which selectively inhibit and activate FSH secretion from the pituitary.
Disease States
Diminished secretion of LH or FSH can result in failure of gonadal function (hypogonadism). This condition is typically manifest in males as failure in production of normal numbers of sperm. In females, cessation of reproductive cycles is commonly observed.
Elevated blood levels of gonadotropins usually reflect lack of steroid negative feedback. Removal of the gonads from either males or females, as is commonly done to animals, leads to persistent elevation in LH and FSH. In humans, excessive secretion of FSH and/or LH most commonly the result of gonadal failure or pituitary tumors. In general, elevated levels of gonadotropins per se have no biological effect.
Pharmacologic Manipulation of Gonadotropin Secretion
Normal patterns of gonadotropin secretion are absolutely required for reproduction, and interfering particularly with LH secretion is a widely-used strategy for contraception. Oral contraceptive pills contain a progestin (progesterone-mimicking compound), usually combined with an estrogen. As discussed above, progesterone and estrogen inhibit LH secretion, and oral contraceptives are effective because they inhibit the LH surge that induces ovulation.
Another route to suppressing gonadotropin secretion is to block the GnRH receptor. GnRH receptor antagonists have potent contraceptive effects in both males and females, but have not been widely deployed for that purpose.
Updated 2018. Send comments to Richard.Bowen@colostate.edu
A Hungarian translation of this page was created by Elana Pavlet and is available at Hungarian translation
A Ukrainian translation of this page was created by Olena Chervona and is available at Ukrainian translation

